They Built a Life in English. Dementia Undid It.
The double exile facing 115,000 Australian elderly migrants

Migration is, at its core, a linguistic act.
You leave one world of words and enter another. You spend years-sometimes decades rebuilding yourself in a new language. Your accent softens. Your vocabulary expands. You start dreaming in English.
Then dementia reverses the entire journey.
For thousands of migrants across Australia, dementia doesn’t just erode memory. It erodes the language they rebuilt their lives around.
English, which is learned, practised, mastered over decades, fades. What remains is the mother tongue. The language of childhood. The one thing their Australian-born children may barely understand.
This is the double exile: first from a homeland, then from the language that replaced it.
The Numbers Behind The Silence
Australia ranks among the most linguistically diverse countries on earth. Over 28 percent of Australians living with dementia come from culturally and linguistically diverse backgrounds. By 2023, an estimated 411,100 people were living with the condition nationally.
Run the numbers: that’s over 115,000 people potentially navigating dementia in a language their healthcare providers don’t speak.
Yet most dementia care infrastructure assumes English: Assessment tools. Care plans. Daily interactions. The entire system rests on a linguistic foundation that crumbles for a significant portion of the people it serves.
What The Brain Does and Undoes
Neuroscience explains the pattern clearly. Dementia erodes recently acquired skills first. Language learned in adulthood, no matter how fluen, sits in a more vulnerable cognitive layer than the mother tongue, which is encoded earlier and deeper.
The result is a cruel reversal. A man who spent fifty years as an English-speaking engineer in Perth wakes up speaking only Italian. His wife, also Italian-born, might still understand. His children, raised in English-speaking schools, might not. His doctor almost certainly doesn’t.
Suddenly, the most basic acts of care like explaining pain, understanding medication instructions, expressing fear require translation. And translation requires resources that are perpetually scarce.
The Interpreter Gap
Professional interpreters remain the gold standard for cross-language healthcare. But the reality falls short of the ideal.
Dementia-trained interpreters are rare. Scheduling takes time that acute care situations don’t allow. And interpreters can’t be present for the hundreds of small daily interactions that constitute life with dementia: the morning greeting from a nurse, the confused request at 4 a.m., the attempt to describe a headache to a care aide.
These micro-moments matter. Research shows that language-sensitive dementia care reduces patient distress, improves diagnostic accuracy, and lowers caregiver burnout. Every interaction that falls through the language gap is a missed opportunity for connection and care.
How Can We Solve This?
This is the space where real-time AI conversation tools make the biggest difference. Not replacing interpreters, but covering the vast territory between scheduled appointments.
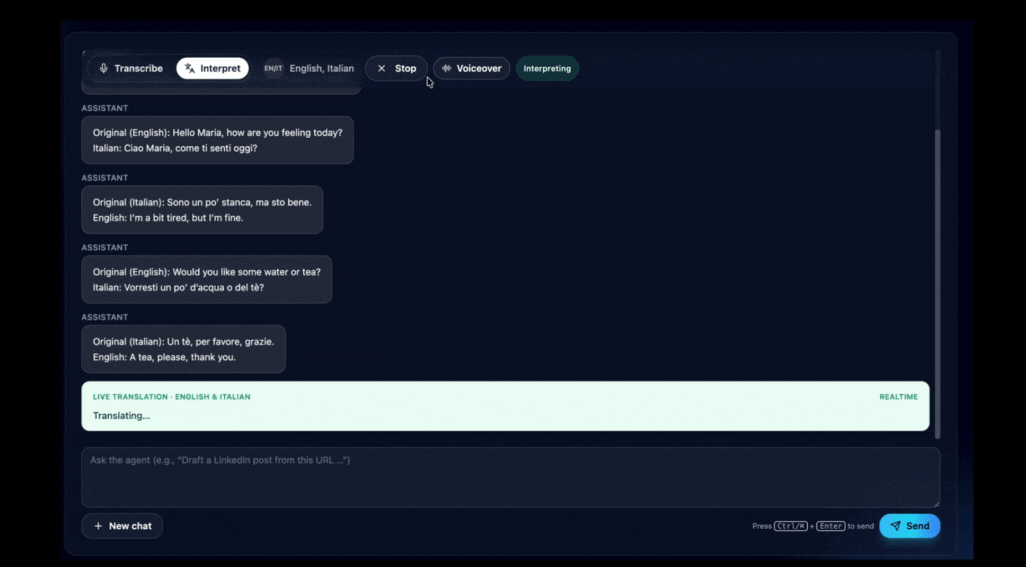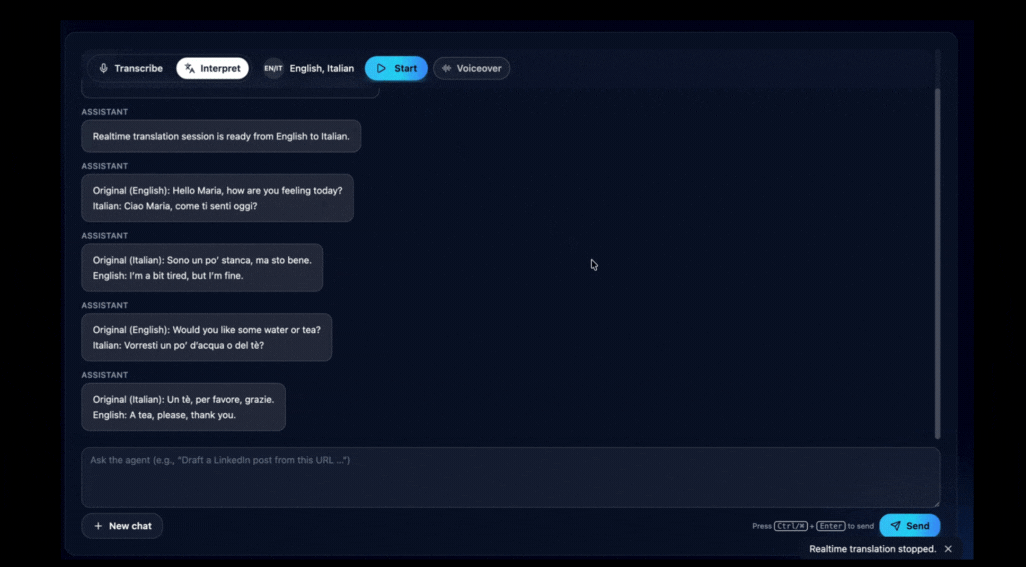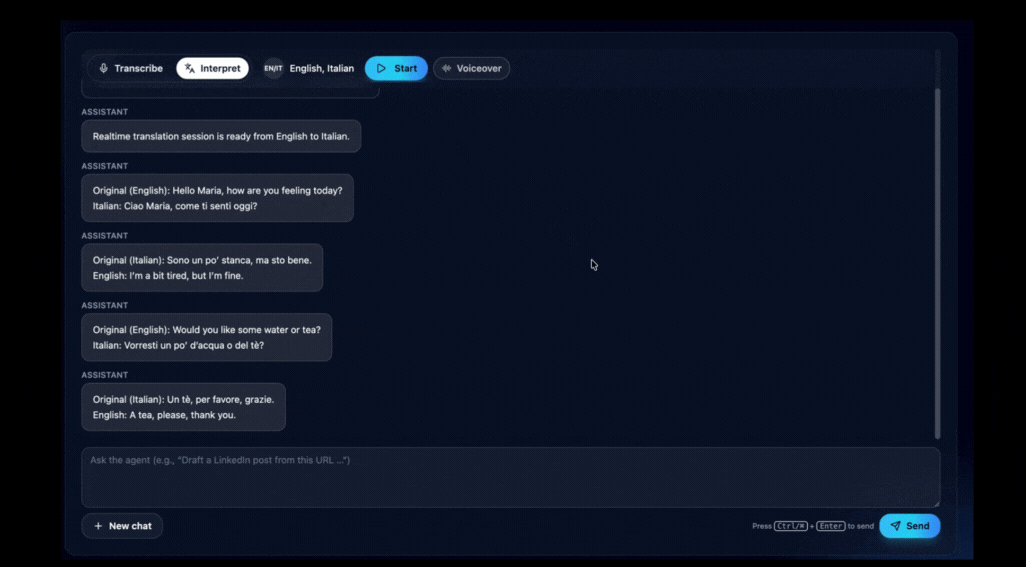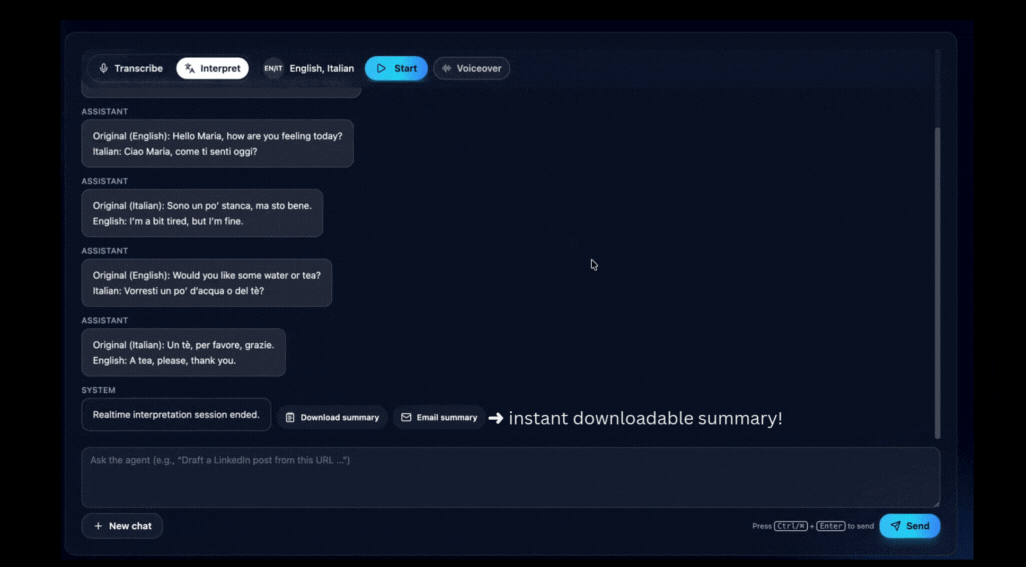
VideoTranslatorAI’s real-time conversation tool interprets live speech across 120+ languages and summarises key points as the conversation unfolds. No downloads, no setup beyond a browser and internet connection.

Illustration: How VideoTranslatorAI’s interpreter works.
In practice, this means a care worker can conduct a bedside check-in with a patient who now speaks only Cantonese and understand them in real time.
A family member joining a specialist consultation can follow along even when their parent switches to a language they barely know.
After the conversation ends, an AI-generated summary captures what was discussed: symptoms reported, concerns raised, and instructions given.
For overstretched care facilities, this isn’t a luxury. It’s infrastructure.
From Add-on to Foundation
Australia has bright spots. Dementia Support Australia provides translated materials and arranges interpreter services.
Victoria’s “language buddies” program pairs isolated individuals with volunteers who share their language. Bilingual cognitive assessments grow more common each year.
But these efforts still treat linguistic diversity as a special accommodation, something bolted onto an English-first system. The shift that’s needed is foundational: designing care systems that expect multilingual patients from the start.
Real-time interpretation and summarisation tools make this practical. When multilingual support is instant and embedded (not booked, scheduled, and budgeted separately), it stops being an exception and starts being the default.
The Words That Remain
Here is what makes this story both heartbreaking and strangely beautiful: the language dementia preserved is the most intimate one. The first words a person ever learned. The sounds of parents, siblings, childhood streets.
The loss isn’t that someone reverts to their mother tongue. The loss is that the world they live in now can’t meet them there.
Closing that gap with trained interpreters, culturally informed care, and technology that works in real time isn’t just good policy. It’s basic human decency.
No one should face dementia in a language the people around them can’t understand.



